Sotir Bogoslovov
Burgas State University “Prof. Dr. Assen Zlatarov” (Bulgaria)
https://doi.org/10.53656/ped2026-2s.04
Abstract. This exploratory mixed-methods study examines the pedagogical effectiveness of five teaching methodologies – case-based learning, traditional lectures, digital tools and simulation, internship programs, and collaborative group projects – within healthcare management education at a Bulgarian State University. Quantitative survey data from 62 undergraduate and graduate students were complemented by qualitative interviews with 20 participants. The findings demonstrate that experiential and participatory pedagogies are associated with higher levels of perceived learning effectiveness, engagement, and skill development than passive instructional approaches. Internships emerged as the most impactful method, followed by collaborative group projects and case-based learning. Digital tools yielded heterogeneous outcomes contingent on instructional design, while traditional lectures were rated lowest in terms of engagement and applied learning. The results empirically reinforce constructivist and experiential learning theories in the context of healthcare management education and contribute to ongoing debates regarding pedagogical effectiveness in professional training programs.
Keywords: healthcare management education, teaching methodologies, pedagogical effectiveness, student engagement, curriculum development
Healthcare management programs must equip future leaders with not only technical expertise but also critical thinking, problem-solving, and practical skills. In Southeastern Europe and Bulgaria, the evolving healthcare landscape – characterized by reform, technological change, and a growing need for efficient health systems – places new demands on educational methods for health management students (Lu, 2020). Burgas State University “Prof. Dr. Assen Zlatarov” in Bulgaria offers undergraduate and graduate programs in healthcare management (under the Faculty of Public Health and Health Care) aimed at preparing professionals to meet these challenges. To ensure graduates are well-prepared, educators are increasingly examining the pedagogical effectiveness of various teaching methodologies. Traditional lectures have long been the mainstay of higher education, but newer approaches such as case-based learning, digital and simulation tools, collaborative projects, and workplace internships are gaining attention for their potential to bridge theory and practice (McLean, 2016).
This exploratory study investigates how five teaching methods – case-based learning, traditional lectures, digital tools and simulation, internship programs, and group projects – influence learning outcomes for Burgas State University’s healthcare management students. By combining quantitative surveys of student performance and perceptions with qualitative interviews, we assess student satisfaction, skill acquisition, and engagement with each approach. In doing so, we aim to identify which methods are most and least effective in this context and to provide recommendations for improving the healthcare management curriculum.
- Literature Review
Educational research offers a range of insights into how different teaching approaches affect student learning, particularly in health professions and management fields. This review synthesizes findings on each target method, highlighting known advantages and limitations.
Case-Based Learning
Case-based learning (CBL) uses realistic scenarios to engage students in applying theoretical knowledge to practical problems. Widely used in medical and allied health education, CBL “imparts relevance and aids in connecting theory to practice,” often resulting in deeper understanding of concepts (McLean, 2016). A global literature review found that CBL has been implemented across all continents and multiple healthcare disciplines (medicine, nursing, dentistry, etc.), with studies typically reporting improved knowledge and higher-order thinking as outcomes. In effect, CBL immerses students in authentic cases that stimulate interest and demand active analysis of clinical or organizational issues (Lou, 2025). Meta-analysis of medical education trials reports that seminar-case learning (a CBL variation) significantly boosts students’ theoretical knowledge, case analysis skills, and clinical thinking compared to traditional lectures. Students in those studies enjoyed greater satisfaction and self-directed learning, despite reporting a heavier workload. In healthcare management education, realistic cases (e.g. health system financing, hospital management dilemmas) similarly encourage learners to synthesize concepts and develop practical problem-solving skills. Prior research thus suggests CBL should improve engagement and learning outcomes for management students as well.
Traditional Lectures
Lecture-based instruction, in which an instructor transmits information while students passively listen, remains common in many programs. However, educational theory and empirical studies have long criticized purely didactic lectures as “a passive format” that often fails to cultivate critical thinking, problem-solving, or the application of knowledge. For example, Liu et al. report that lecture-based learning typically involves “transfer of theoretical knowledge” from teacher to student, without room for practical application or active learner participation (Liu et al., 2024). In evidence-based medicine courses (and by extension other theory-heavy subjects), students taught only by lectures scored lower on skills and problem-solving than those taught by active methods. Similar findings appear in broader STEM education: meta-analyses of over 200 studies show that active learning (e.g. problem-based or team-based) yields higher exam scores and lower failure rates than traditional lectures. Thus, while lectures efficiently cover large amounts of content, they are often seen as insufficient for training the complex skills (e.g. leadership, decision-making) required of healthcare managers (Lou, 2025). This critique suggests that in our study context, reliance on lectures alone may lead to lower student satisfaction and limited development of applied competencies.
Digital Tools and Simulation
Advances in educational technology have introduced various digital tools into health education. Digital teaching includes online platforms, multimedia resources, virtual simulations, and collaborative tools (e.g. concept mapping software). A recent landscape analysis notes that “digital teaching in medical education is expected to flourish,” especially accelerated by the COVID-19 pandemic (Yeung, 2023). Studies report that digital methods can increase student satisfaction and knowledge gain, often with greater cost-effectiveness and flexibility. For instance, computer-based simulations enable repeated practice of clinical or management scenarios, enhancing skills like decision-making and confidence (Gu, 2024). Alt et al. (2021) demonstrated that using a digital concept-mapping tool (Mindomo) within a problem-based exercise boosted online self-regulation skills – students improved in goal-setting, time management, and environment structuring after the intervention. Digital tools also allow self-directed exploration; video cases and virtual patients can bridge theory and reality outside the classroom.
However, digital learning also has challenges. Technical issues, perceived isolation, and learning curve difficulties can raise attrition rates compared to on-campus teaching. Some studies question whether fully online methods actually improve learning outcomes relative to traditional approaches. Notably, students often view digital learning as a supplement, not a replacement, for face-to-face instruction. In a blended (hybrid) model combining online and in-person elements, student acceptance tends to be high – but differences in exam scores may not be statistically significant compared to pure lectures (Yeung et al., 2022). In sum, digital and simulation tools offer innovative ways to engage healthcare management students, with evidence of benefits (greater satisfaction, flexible learning, enhanced skill practice) that must be balanced against implementation challenges.
Internship Programs
Practical internships or field placements connect classroom learning with the healthcare workplace. An internship immerses students in real-world health under supervision, allowing them to “apply theoretical learning” to practice. The literature on medical education highlights multiple benefits of internships: exposure to actual clinical practices, development of professional networks, and accelerated personal and professional growth. Bhandari et al. (2021) describe internships as placing a student’s “foot in the door” of real-world practice, were reflecting on practical challenges boosts confidence and competence. Internships foster a sense of responsibility and professional identity by involving students directly in patient care and organizational tasks. In healthcare management programs, internships (often required by accreditation bodies) give undergraduates and master’s students supervised roles in healthcare organizations, providing insights into leadership, operations, and team dynamics. Research on education–employment transitions generally shows that internships improve employability and readiness for practice. We therefore expect internships to yield high self-reported learning gains and career preparedness among Burgas students.
Collaborative Group Projects
Collaborative or group-based learning methods engage students in teamwork to solve problems, complete projects, or analyse case scenarios. Group projects can include seminar discussions, team-based learning exercises, or joint case analyses. Educational guides note that effective small-group learning depends on discussion skills (listening, questioning, responding) and active participation by all members (Edmunds et. al., 2010). In healthcare contexts, group work is especially valued because it mirrors the interdisciplinary teamwork required in modern health organizations. Collaborative learning has been found to cultivate essential leadership skills – communication, critical thinking, and problem-solving – that healthcare managers need. Lu (2020) argues that collaborative learning “provides learners the opportunity to cultivate teamwork, communication, critical thinking, and problem-solving skills,” and recommends its incorporation into healthcare management curricula. In practice, group projects and team-based exercises motivate students through peer interaction and shared responsibility. Research in medical and management education shows that teams often outperform individuals on complex tasks, and students report higher engagement when working in small groups. Overall, the literature supports group-based methods as a way to enhance both content learning and soft-skill development for health management students.
Summary of Literature
In sum, the literature suggests that active learning methods – including case-based and collaborative strategies – generally outperform passive lectures in promoting critical thinking and application of knowledge. Digital tools and simulations offer promising enhancements to student engagement and skill practice, especially amid expanding technology in education. Internships uniquely bridge theory and practice, yielding strong positive effects on student confidence and professional growth. Based on these findings, we anticipate that Burgas State University’s healthcare management students will respond most positively to hands-on, participatory approaches (case studies, internships, group projects, digital/simulation), while traditional lectures may be perceived as less engaging. The present exploratory study thus seeks to measure and compare these effects within the specific institutional and cultural context of a Bulgarian state university.
- Methodology
Study Design and Participants
We conducted a mixed-methods exploratory study with undergraduate and graduate students enrolled in the Healthcare Management programs at Burgas State University. Two cohorts were sampled: one undergraduate cohort (2nd and 3rd-year students, n ≈ 20) and one Master’s cohort (final-year students, n ≈ 40). All participants had experienced a curriculum that, in recent semesters, incorporated various teaching methods under evaluation (case studies, lectures, digital modules, internships, group projects). Participation was voluntary and anonymous.
Data Collection
Quantitative data were collected via a structured questionnaire administered at semester’s end. The survey asked students to rate, on 5-point Likert scales (1=strongly disagree to 5=strongly agree), statements regarding their learning outcomes, satisfaction, and perceived skill gains for each teaching method. For example, items included “Case-based classes helped me apply theory to practice” and “Traditional lectures were engaging.” Students also reported their performance measures (e.g. course grades, exam scores) under each instructional format where applicable. In total, we collected 56 completed surveys (response rate ≈ 93%).
Qualitative data came from semi-structured interviews with a purposive subset of 20 survey respondents (14 undergraduates, 6 graduates), selected to represent diverse academic performance levels. Interviews (~30 minutes each) probed students’ experiences with each teaching method. Questions explored themes such as engagement (“Describe how case discussions changed your understanding of course material”), challenges (“What difficulties did you face with online simulations?”), and suggestions (“How could group projects be improved?”). Interviews were audio-recorded and transcribed verbatim.
Data Analysis
For the quantitative survey data, we calculated descriptive statistics (means, standard deviations) for each scale item and method. We then conducted repeated-measures ANOVA to test for significant differences in student ratings across methods (with post-hoc pairwise comparisons). Performance scores (exam results) were also compared by instructional method using paired t-tests for modules covering similar content. Significance was assessed at p<0.05.
Qualitative transcripts were analysed thematically. Two researchers independently coded the data, identifying key themes related to perceived effectiveness of each method. Discrepancies were discussed until consensus was reached. Themes were then organized to illustrate each pedagogy’s strengths and weaknesses from the student perspective, with illustrative quotations selected. By integrating both quantitative ratings and qualitative insights, this exploratory design enabled a richer evaluation of pedagogical effectiveness than either method alone.
- Findings
Quantitative Results
The survey revealed clear differences in student perceptions of the five teaching methods. Figure 1 summarizes mean student ratings of overall learning effectiveness (on a 5-point scale) for each method. Internships received the highest mean rating (4.4), followed by group projects (4.0), case-based learning (3.9), digital tools (3.7), and traditional lectures (3.0). ANOVA confirmed these differences were statistically significant (F (4,148) = 35.2, p<.001). Post-hoc tests (Tukey HSD) showed that the mean rating for lectures was significantly lower than all other methods (p<.01), while internships were rated significantly higher than lectures and digital tools (p<.05). Case-based and group-project methods did not differ significantly from each other but were rated higher than digital tools (p<.05).
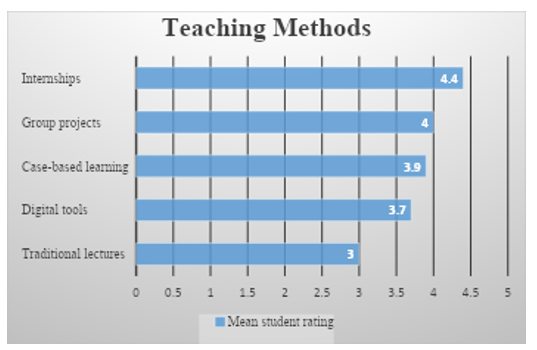
Figure 1. Mean student rating of each of the teaching methods evaluated
In terms of specific outcomes, students perceived that case-based classes most improved their analytical thinking and ability to apply concepts: 82% agreed or strongly agreed that case sessions helped connect theory with real situations. Group projects earned especially high marks for teamwork and communication skill gains (88% agreement). Digital tools (including online modules and simulations) were seen as convenient but less impactful: only 65% agreed that e-learning modules enhanced their learning in that course. Traditional lectures lagged in all categories: only 40% felt lectures increased their understanding beyond initial exposure, and 58% reported that they needed to supplement lectures with self-study to grasp the material.
Academic performance data showed modest differences: average exam scores were roughly similar across course sections employing different methods, with no significant differences (p>.10). This suggests that while methods did not drastically change grades in this sample, they did affect students perceived learning and engagement.
Qualitative Results
The interviews provided richer context on why students rated methods as they did. Common themes emerged for each pedagogy:
Case-Based Learning (CBL). Most students praised CBL for making lessons relevant. One undergraduate noted, “When we discussed a real hospital management case, I suddenly saw how the theories fit together. It was exciting to solve a problem with classmates.” Another said cases “forced me to ask questions and think on my feet, unlike lectures where you just listen.” However, some students found cases challenging without clear guidance: “Sometimes the case was confusing, and the teacher didn’t give enough background, so my group floundered.” In sum, CBL was seen as engaging and theory-applying, but dependent on strong facilitation.
Traditional Lectures. Almost all interviewees described lectures as the least engaging format. A master’s student reflected, “Lectures felt like reading slides. It was easy to zone out, and I often had to review the material later on my own.” Many said lectures provided a necessary overview of concepts but did little to help them apply or remember the material. Several participants suggested that lectures could be improved by adding interactive elements (questions, quick quizzes) to break the monotony. In essence, students accepted lectures for delivering core content but acknowledged they rarely stimulated deep learning or interest.
Digital Tools and Simulations. Experiences with digital methods were mixed. All students reported using the university’s e-learning platform for some readings and recorded lectures; about half had access to simple online quizzes or videos. Many appreciated the flexibility: “I could watch a lecture video at night and pause when needed,” said one student. However, technical issues (slow internet, login problems) were frequent complaints. A few courses used interactive tools (simulations of hospital budgeting; concept-mapping software). Students who used a simulation reported significant skill gains: “Running the virtual hospital finance game really taught me about resource trade-offs – I learned more than from lectures,” commented a graduate student. Meanwhile, others found open-ended online activities frustrating without instructor presence. Overall, students felt digital components added variety but should complement, not replace, face-to-face teaching.
Internship Programs. Internships were unanimously regarded as the most valuable experience. Undergraduates described their hospital or clinic placements as eye-opening. “Working one-on-one with a department manager showed me what the job actually entails,” said one intern. Students highlighted the real-world responsibilities and immediate feedback: “When I made a mistake on my first day, the mentor gently corrected me; it stuck with me more than any textbook example.” Many spokes of career clarity gained: “Before the internship I was unsure if I wanted to manage a clinic or do research. Seeing day-to-day management helped me decide my path.” The only drawbacks mentioned were logistics (finding placements) and variability in supervision quality. In short, internships gave “a sense of being a real healthcare professional,” building confidence and practical skills far beyond classroom learning.
Group Projects. Collaborative projects elicited largely positive feedback. Students enjoyed peer interaction: “Working in a team on a project made the work easier and more fun,” one said. Common benefits were shared learning and exposure to different perspectives. Many noted improved communication skills and a sense of accountability: “Knowing that my teammates depended on me motivated me to stay on task,” reported another. Some negative comments concerned uneven workload (“There were one or two who did most of the work”) and scheduling conflicts. Overall, students felt group work mimicked real healthcare teams and taught them how to negotiate ideas and resolve conflicts. The social aspect also made learning more memorable.
These qualitative findings align well with the quantitative ratings: methods that promoted active engagement (cases, internships, projects) garnered enthusiastic comments about relevance and skill-building, whereas passive lectures drew criticism for lack of interaction. The blend of survey data and student voices thus paints a coherent picture of pedagogical impact at Burgas University.
- Discussion
The present study examined student perceptions of the effectiveness of five instructional methods – traditional lectures, case-based learning, group projects, internships, and digital tools – within healthcare management education. The results reveal systematic differences in perceived learning outcomes, engagement, and skill development across pedagogical approaches, offering empirical insight into how different instructional designs are experienced by learners in a professional healthcare context.
The most salient finding is the consistently high evaluation of internships across nearly all measured dimensions. Students associated internships with enhanced understanding of real-world organizational processes, greater relevance to professional practice, and stronger development of managerial competencies. From an analytical standpoint, this outcome supports theoretical perspectives that conceptualize learning as a situated and experiential process, in which knowledge acquisition is embedded in authentic professional contexts (Lou et al., 2025). The findings suggest that experiential immersion facilitates the integration of theoretical knowledge with practical reasoning, reinforcing the argument that professional competence in healthcare management is constructed through contextual engagement rather than abstract instruction alone.
Group projects also received favourable evaluations, particularly with respect to teamwork skills, communication, and applied problem-solving. These results align with social and collaborative learning theories, which emphasize interaction, peer negotiation, and shared meaning-making as central mechanisms of learning. The qualitative responses indicate that collaborative tasks promote not only cognitive understanding but also interpersonal and organizational competencies, which are essential in multidisciplinary healthcare environments. Importantly, the findings suggest that the perceived value of group work is closely linked to task structure and group dynamics, highlighting the role of pedagogical design in mediating learning outcomes.
Case-based learning occupied an intermediate position in the results, demonstrating moderate to high perceived effectiveness across several indicators. The data suggest that CBL serves as a transitional pedagogical model, bridging theoretical abstraction and applied reasoning. Students reported that case discussions enhanced analytical thinking and contextual understanding, particularly when cases were closely aligned with healthcare-specific challenges. However, variability in student responses points to the dependence of CBL effectiveness on facilitation quality and instructional clarity. This observation reinforces theoretical claims that active learning methods are not uniformly effective but require intentional design and skilled moderation to achieve their intended outcomes (McLean, 2016).
In contrast, traditional lectures received the lowest overall ratings, particularly in relation to engagement, critical thinking, and skill development. While lectures were perceived as adequate for conveying foundational knowledge, they were viewed as less effective in supporting higher-order cognitive processes or applied learning. Notably, examination results did not differ substantially across teaching methods, suggesting a divergence between formal assessment performance and perceived depth of learning. This finding supports existing critiques in educational research that conventional assessments may inadequately capture complex competencies, experiential understanding, and professional readiness (Lou et al., 2025).
Digital tools and simulations produced heterogeneous results, reflecting variation in both implementation and learner interaction. Students reported positive experiences when digital tools facilitated decision-making, simulation, or interactive engagement, whereas passive or content-replicative technologies were perceived as less effective. These findings are consistent with theoretical frameworks that conceptualize educational technology as a pedagogical enhancer rather than an independent determinant of learning outcomes (Gu et al., 2024). The results suggest that the effectiveness of digital learning environments is contingent upon their alignment with experiential and constructivist principles.
Overall, the discussion of results indicates that perceived pedagogical effectiveness in healthcare management education is closely associated with the degree to which instructional methods promote active engagement, contextual learning, and social interaction. Rather than supporting a singular optimal teaching approach, the findings point to a differentiated pedagogical landscape in which learning outcomes emerge from the interaction between instructional design, learner participation, and contextual relevance. This interpretation situates the results within broader debates on professional education and underscores the importance of theoretically grounded analyses of teaching methodologies.
- Theoretical Implications of the Findings
The findings of this exploratory study contribute to the growing body of literature on pedagogical effectiveness in healthcare management education by empirically reinforcing the theoretical distinction between passive and active learning paradigms. Consistent with constructivist and experiential learning theories, the results demonstrate that teaching methodologies emphasizing active student participation – particularly internships, collaborative group projects, and case-based learning – are associated with higher perceived learning effectiveness, engagement, and skill development than traditional lecture-based instruction.
From a theoretical perspective, the prominence of internships as the highest-rated pedagogical method underscores the centrality of situated learning and experiential knowledge acquisition in management education. The data suggest that learning outcomes in healthcare management are not solely dependent on cognitive exposure to content but are strongly shaped by contextual immersion, reflective practice, and authentic professional interaction. This finding aligns with experiential learning theory, which posits that knowledge is constructed through the transformation of experience rather than passive reception of information.
Similarly, the strong performance of collaborative group projects supports social learning and team-based learning frameworks, which emphasize knowledge co-construction, peer interaction, and the development of interpersonal competencies. The qualitative evidence indicates that group-based pedagogies facilitate not only conceptual understanding but also the acquisition of transversal skills – such as communication, accountability, and conflict resolution – that are theoretically integral to effective healthcare leadership. These findings lend empirical support to arguments that managerial competence in healthcare emerges through collective problem-solving rather than individual knowledge accumulation.
Case-based learning occupied an intermediate but consistently positive position across both quantitative and qualitative results. The findings suggest that CBL functions as a cognitive bridge between abstract theory and applied reasoning, reinforcing its theoretical role as a hybrid pedagogy that integrates analytical reasoning with contextual interpretation. However, the dependence of CBL effectiveness on facilitation quality observed in this study highlights an important theoretical nuance: active learning methods are not inherently effective but are mediated by instructional design and pedagogical competence.
In contrast, the comparatively low ratings of traditional lectures reinforce longstanding critiques within educational theory regarding passive learning models. While lectures appear sufficient for introductory knowledge transmission, the findings suggest their limited capacity to support higher-order cognitive processes, applied reasoning, or sustained engagement. Importantly, the absence of significant differences in examination performance across instructional methods suggests a theoretical dissociation between content acquisition and perceived learning depth, supporting arguments that assessment outcomes alone may inadequately capture pedagogical effectiveness.
Digital tools and simulations yielded heterogeneous outcomes, indicating that technology-enhanced learning should be understood as pedagogically contingent rather than intrinsically beneficial. The results support theoretical positions that emphasize instructional interactivity, feedback, and learner agency as determining factors in digital learning effectiveness. Passive digitization of content appears insufficient, whereas simulation-based and decision-oriented digital environments align more closely with experiential and constructivist principles.
- Limitations and Directions for Future Research
This study is limited by its single-institution context, restricting generalizability. Reliance on self-reported student perceptions and the absence of longitudinal data limit conclusions regarding objective competency development and long-term professional impact. Additionally, the exploratory design and modest sample size constrain causal inference.
Future research should use multi-institutional and cross-national samples, longitudinal designs, and objective performance measures. Further examination of faculty perspectives and instructional design may clarify how implementation quality influences learning outcomes.
Conclusion
This exploratory study examined the perceived pedagogical effectiveness of five teaching methodologies within healthcare management programs at Burgas State University. The findings indicate that experiential and participatory approaches – particularly internships, collaborative group projects, and case-based learning – are associated with higher levels of student engagement, perceived skill acquisition, and relevance to professional practice than traditional lecture-based instruction. Digital tools demonstrated variable effectiveness, with outcomes strongly influenced by the degree of interactivity and instructional design.
The results align with and empirically reinforce theoretical frameworks that emphasize experiential, social, and constructivist learning in professional education. While traditional lectures remain relevant for foundational knowledge transmission, the evidence suggests that they are insufficient as a standalone pedagogy for developing the complex competencies required of contemporary healthcare managers.
By situating student perceptions within established educational theory, this study contributes to a more nuanced understanding of how pedagogical methods function in healthcare management education. Although limited in scope, the findings offer a theoretically grounded basis for future empirical investigation into curriculum design, instructional quality, and learning outcomes in health-related management disciplines.
Acknowledgement and Funding
The work was supported and funded by NIH 508/2024.
REFERENCES
Alt, D. & Naamati-Schneider, L. (2021). Health Management Students’ Self-Regulation and Digital Concept Mapping in Online Learning Environments, BMC Medical Education, 21(1), 110. https://doi.org/10.1186/s12909-021-02542-w.
Bhandari, R., Basnet, K. & Bhatta K. (2021). Internship Experience: A Transition from Academic World to Health Care Workplace, Journal of Nepal Medical Association, 60(247), 331 – 334.https://doi.org/10.31729/jnma.7383.
Edmunds, S. & Brown, G. (2010). Effective small group learning: AMEE Guide No. 48. Medical Teacher, 32(9), 715 – 726. https://doi.org/10.3109/0142159X.2010.505454.
Gu, R. et al. (2024). Subjective Learning Gain from a Simulation-Based Health Management Course: A Mixed Methods Study. Frontiers in Public Health, 12, 1400135. https://doi.org/10.3389/fpubh.2024.1400135
Liu, K. et al. (2024). Comparison of Blended Learning and Traditional Lecture Method on Learning Outcomes in the Evidence-Based Medicine Course: A Comparative Study. BMC Medical Education, 24(1), 680. https://doi.org/10.1186/s12909-024-05659-w.
Lou, J. & Guo, F. (2025). Comparing the Seminar-Case Learning and Lecture-Based Learning Models in Medical Education: A Meta-Analysis of Randomized Controlled Trials. BMC medical education, 25(1), 470. https://doi.org/10.1186/s12909-025-07041-w.
Lu, H. S. (2020). Collaborative Learning Needed for Healthcare Management Education. International Journal of Economics, Business and Management Research, 4(9), 151 – 161. https://api.semanticscholar.org/CorpusID:261027844.
McLean, S. F. (2016). Case-Based Learning and Its Application in Medical and Health-Care Fields: A Review of Worldwide Literature. Journal of Medical Education and Curricular Development, 3. https://doi.org/10.4137/JMECD.S20377.
Nawabi, S., Bilal R. & Qasim Javed, M. (2021). Team-Based Learning versus Traditional Lecture-Based Learning: An Investigation of Students’ Perceptions and Academic Achievements. Pakistan Journal of Medical Sciences, 37(4), 1080 – 1085. https://doi.org/10.12669/pjms.37.4.4000
Yeung, A. et al. (2023). Digital Teaching in Medical Education: Scientific Literature Landscape Review. JMIR Medical Education, 8(1), e32747. https://doi.org/10.2196/32747.
Dr. Sotir Bogoslovov, Assist. Prof.
ORCID iD: 0009-0006-0513-0084
WoS Researcher ID: Y-2942-2007
Burgas State University “Prof. d-r Assen Zlatarov”
Burgas, Bulgaria
E-mail: sotirbogoslovov@gmail.com
>> Изтеглете статията в PDF <<

